

When it comes to breaking news for you the fastest and in the most comprehensive and accurate manner, be it from Odisha or beyond, OdishaTV is the best

Sofia Firdous was present in the meeting amid speculations that she may be picked as the Congress candidate for the seat, as Moquim may not contest the election due to the ORHDC loan scam case. He could not get a stay on the Orissa High Court order pertaining to the case.

The district administration organised an awareness drive in Baliguda of Kandhamal district for voters. A fashion show was organised as a part of the drive during which the sub-collector along with other participants walked the ramp.

BJP president of Sonepur district, Parmod Mohapatra said, "Thousands of party workers from Sonepur, Boudh and Bolangir will come to the public meeting.”

Chief Minister Naveen Patnaik's sudden sartorial leaning towards the lungi, that too before the elections, triggered reactions from BJP leaders on social media, who questioned the motive citing Odia culture, pride and tradition.

The BJP stalwart said, "The people have enthusiasm for the leadership of Prime Minister Narendra Modi. Such huge support indicates that they want to see Narendra Modi as the Prime Minister for the third time. They want a double-engine government in Odisha.”

Launching a salvo at the opposition parties, the Chief Minister, said, “They are maligning the state government. No one has ever been successful by opposing development. The people of Odisha have come to know the true nature of the opposition parties.”

The BJP has issued a chargesheet against the BJD-led government in Odisha, citing various governance failures and corruption allegations ahead of the 2024 elections. Key issues include an electricity pricing scandal, high crime rates against women, cultural heritage destruction, healthcare collapse, and exploitation of farmers and youth.

The sitting Jatani MLA has been in the eye of a storm after his son Manmath Routray was given a BJD ticket to contest from the prestigious Bhubaneswar Lok Sabha seat against BJP’s sitting MP Aparajita Sarangi.
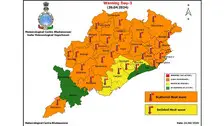
Bhubaneswar experiences severe heat with temperatures crossing 43 degrees Celsius, triggering an IMD-issued orange warning for a severe heat wave across Odisha. No cooling relief is expected soon, with predictions of further temperature increases.

The Odisha Joint Entrance Examination (OJEE) 2024 will be held from May 6 to May 10 in a computer-based format. The exam is for various degree and master's courses, with the application period having ended in March.

Another senior Congress leader said that Sofia is not a new candidate, rather she was involved since 2014 and campaigned for her father in 2019 as well.

The BJP has released a chargesheet against the BJD, highlighting the latter's failures in governance over 25 years in Odisha. The document, influenced by public feedback, points out issues like women's safety, rising crime against children, job scarcity leading to migration, and unfair electricity pricing.

As per the allegations by some residents, they don’t have basic amenities in their area like road communication and drinking water facilities. However, no political party is concerned about their ordeal.

The BJP has issued a 'chargesheet' against the BJD, accusing it of misgovernance during its 25-year tenure in Odisha. Key issues raised include corruption, insufficient welfare measures, and lack of employment. The BJP aims to challenge the BJD in the upcoming 2024 elections, highlighting failures in agriculture and women's safety.

Copyright © 2024 - Odisha Television Limited All Rights Reserved.